The term cellulite refers to the deposition of subcutaneous fat in muscles and tissues under the skin. This fat deposition leads to a bumpy, “dimple-like” appearance on the skin. Cellulite is common in women and usually occurs on the thighs and buttocks. However, it is possible to experience the same effect on the breasts.
What causes cellulite in the breast?
Table of content
Similar to your thighs and buttocks, this area is made up of fat. The anatomy of a woman’s breast constitutes the specialized tissue known as the glandular tissue, as well as the fatty tissue and the ducts that carry the milk to the nipples.
The milk-producing glandular tissues are sectioned into parts known as lobules. There are also connective tissue and ligaments that hold the whole structure together and give your boobs its shape. Unlike the woman, those of a man lacks the milk-producing lobules. However, the male breast has its fair share of adipose tissue.

In 2009, a cellulite severity scale ranked the appearance of cellulite in the form of grades. Grade ‘1’ is the orange peel appearance. Here, the skin exhibits a slightly draped or sagging appearance. Grade 2 is moderate cellulite deposit which gives the skin a cottage skin appearance. Whereas grade 3 is severe, with more than 10 dimples occurring giving the skin a severely draped appearance. When it comes to the breasts, the most common symptom is usually one or two indents or dimples on its skin. Some indentations become noticeable when you lift your arms or flex your muscles.
Fat deposit in the boob area is a possibility, especially in women. About 85% of the cases of cellulite deposit is on women above the age of 20 years. This incidence is usually as a result of genes, and hormones. The fat deposit begins to push through the connective tissue and lobules leading to an “orange peel effect/ Peau D’Orange.” However, the issue with cellulite in breasts is that the condition is mostly associated with cancer, infection, or lymphedema.
a). Breast Cancer leading to cellulite and dimpling
The occurrence of a tumor in the breast can cause skin irritation leading to indentation. This cancer is common in women due to the uncontrollable growth cells in this part. The dimpling effect is a common symptom, along with other symptoms such as:
- Discomfort
- Nipple discharge
- Discoloration of the skin, e.g. breast redness
- Inflammation
- Nipple retraction
For this reason, it is advisable to go for a check-up by a healthcare professional.
b). Breast cellulitis
This is an uncommon condition that can be mistaken for inflammatory breast cancer. This infection usually affects the dermis and subcutaneous tissue of the skin leading to the dimpling effect or dimpled breasts.
It can affect anyone. However, women who are at high risk of developing the condition include breastfeeding mothers, women who have undergone a breast surgery, including women who have experienced chemotherapy. Women who have experienced cancer on this body part have a high risk of developing the condition not only around the time of their surgery but also later on after treatment. This condition is associated with pain, swelling and breast tenderness, along with a sense of warmth.
Cellulitis looks like a breast abscess in that is deforms the skin. However, cellulitis tends to spread around, under the skin without pulling into one pocket like an abscess.
c). Fat necrosis
This condition occurs when a fatty breast tissue gets damaged. A variety of factors can trigger this damage, for instance, a traumatic injury maybe during sports, or after a breast surgery. Fat necrosis often resembles breast cancer. Once the fatty tissue becomes damaged or dies, it develops into a scar tissue and may trigger the formation of a cyst, as well as lump formation. The condition is also known as membranous fat necrosis/post-traumatic pseudolipoma/Liponecrosis microcystica calcificata.
Is breast dimpling always cancer?
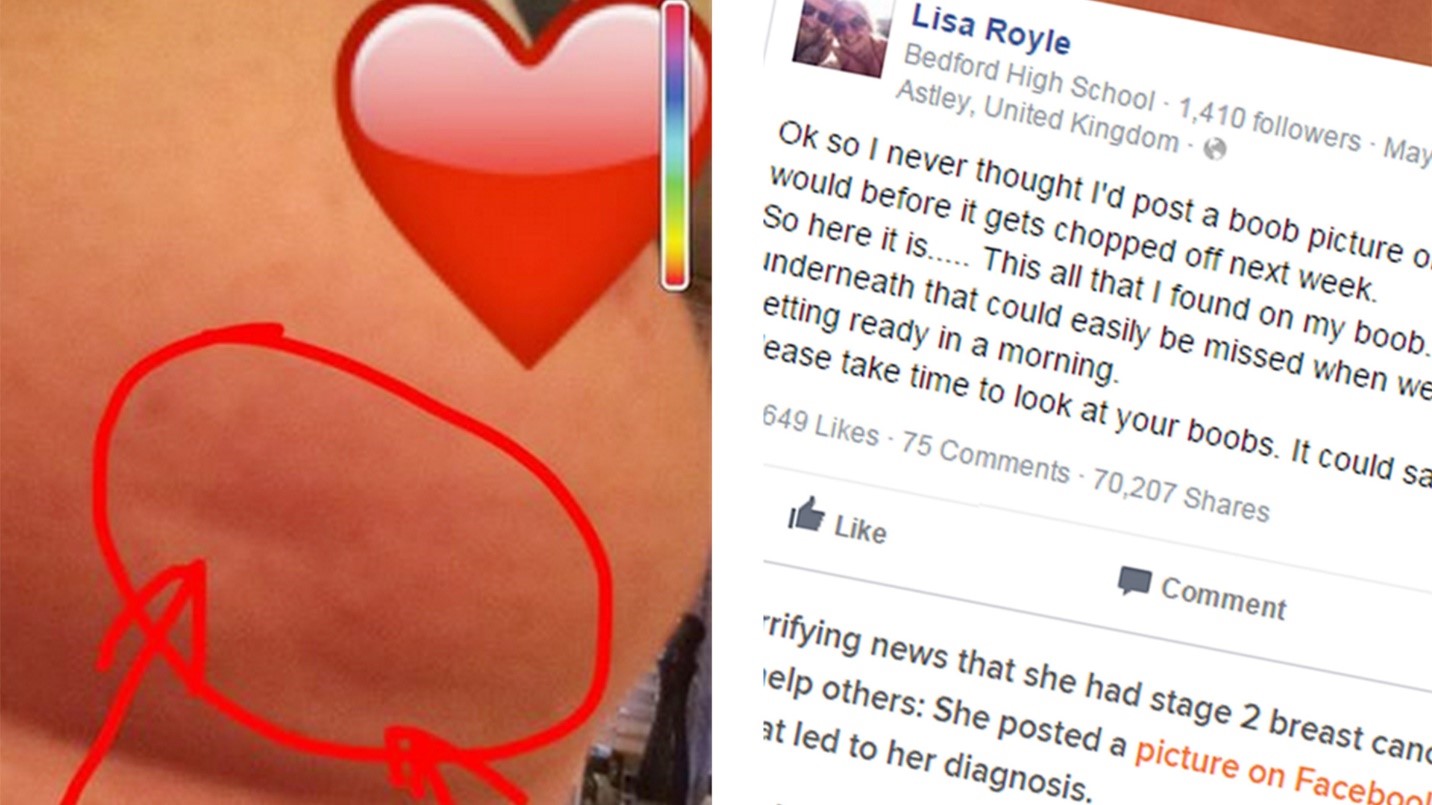
Three years ago, a photo by Lisa Royale of one of her dimpled boobs went viral. The 42-year-old mother posted the photo of her early symptoms of breast cancer to warn other women to check themselves. Indeed, change on this part are a serious issue and cannot be taken lightly.
Alternatively, there are benign cases that could trigger cellulite. One of the most common cases is pregnancy. The hormonal changes that occur during pregnancy can result in extra fat deposit in the breasts. As a consequence, the changes and you may notice some slightly draped appearance.
Also, the weakening of the Cooper ligaments can alter the structure of the female mammary glands giving it that cellulite-like appearance. Women who have had multiple pregnancies repeatedly stretch the skin thereby weakening the cooper ligaments. The repeated enlargement of the breast for lactation, followed by the diminishing milk glands after lactation may trigger the appearance of some dimpling effect on them.
Breastfeeding mothers reduce their chances of getting breast cancer through breastfeeding their babies. Contrary to popular myth, lactating does not lead to sagging. Rather, the breast enlargement during lactation stretches the skin. Once they start to reduce in size, the loose skin can give the appearance of cellulite.
At the same time, it is important to note that there is a combination of factors that may lead to the cellulite appearance. These factors include postpartum hormonal changes, changes in weight, age, and the number of pregnancies.
Treatment and remedies at home
It is important that you go for a check-up to confirm whether the mammary glands changes you are experiencing are benign or a symptom of a medical condition. You will probably have to undergo a series of tests such as a mammogram, ultrasound or biopsy. That said, if you are lucky enough to find out that the cellulite in your breasts is benign, that you can opt for certain lifestyle changes that include regular exercise and healthy eating. There is a lack of substantial evidence citing that skin-firming creams can help reduce cellulite. However, there are some home remedies you can try out to give your breasts a fuller, healthier shape.
References:
- Jo Ann Rosenfeld. Handbook of Women’s Health, Cambridge University Press, 2009
- https://goo.gl/kTqvDa
- https://goo.gl/Vfq9cj
- https://goo.gl/Mc2RXP
- https://goo.gl/rnuQWq
- https://goo.gl/4VnQ3C
- https://goo.gl/Lx1GS9
